Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
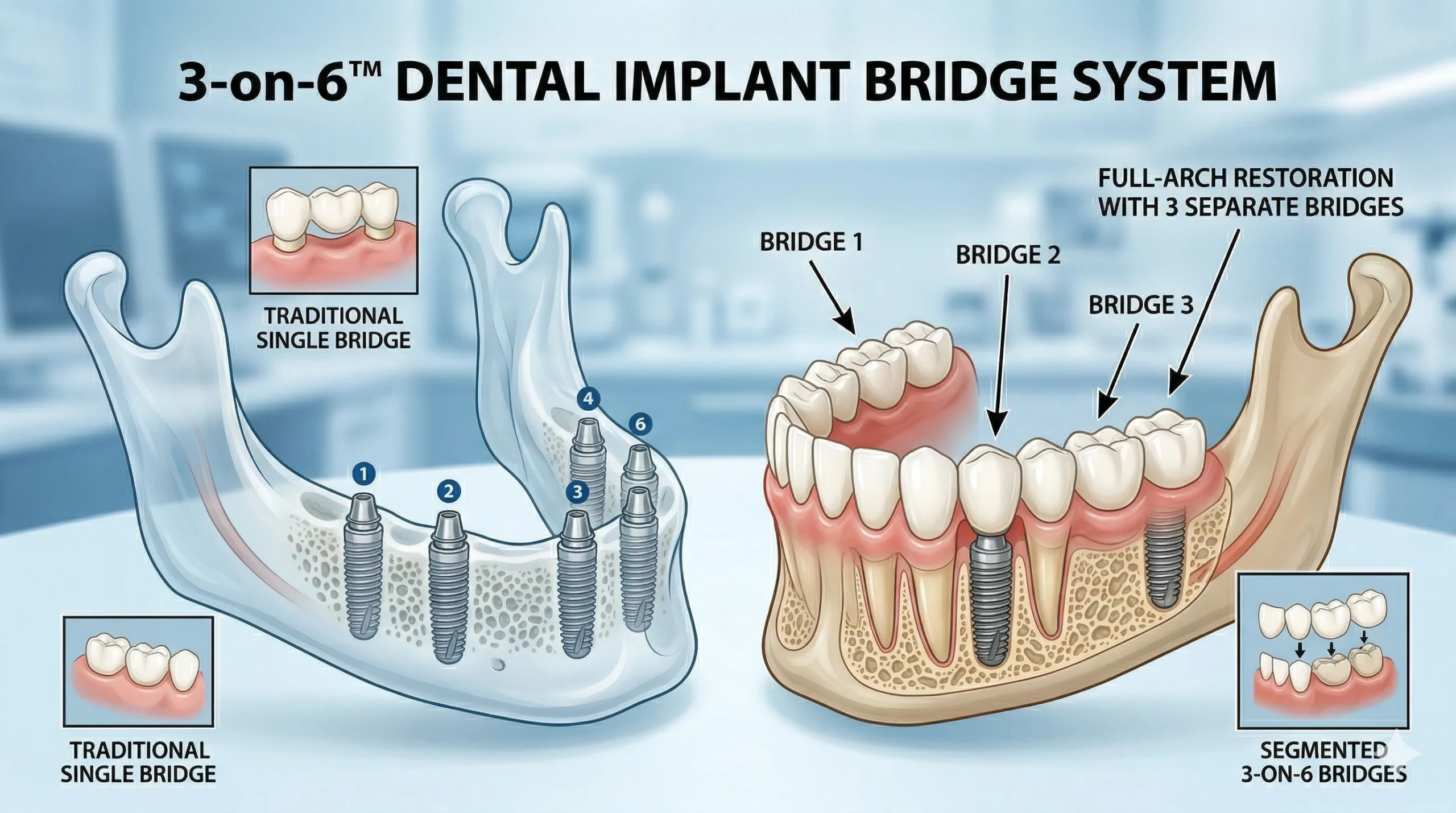
The name describes the structure directly: three bridges supported by six implants. Rather than placing one implant per missing tooth, six titanium posts are positioned strategically across the jaw — typically two at the front and two on each side. Three custom-made bridge sections are then anchored to these posts, collectively replacing all the teeth in a full arch.
The result is a fixed restoration. Unlike removable dentures, it doesn’t come out at night, doesn’t require adhesives, and doesn’t move when you eat or speak. It functions more like natural teeth than any removable alternative.
The six-implant foundation is what distinguishes this approach from options like All-on-4, which uses fewer posts. More implants mean more contact points with the bone, broader load distribution, and generally greater long-term stability — particularly under the pressure of chewing.
Patients exploring full-arch replacement often encounter several options, and it helps to understand where 3-on-6 sits among them.
All-on-4 uses four implants per arch, with the two rear implants angled to avoid areas of lower bone density. It’s a well-established technique and suits patients who have experienced significant bone loss. The tradeoff is that four implants carry more load per post than six, and the angled placement, while effective, isn’t always the most biomechanically ideal arrangement.
All-on-6 adds two more implants to the All-on-4 framework, improving load distribution. 3-on-6 is closely related but differs in the bridgework design — three separate bridge sections rather than a single full-arch prosthetic. This segmented approach can make future maintenance and repairs more straightforward, since individual sections can be addressed without disturbing the entire restoration.
Removable implant-supported dentures use implants as anchors but the prosthetic itself can be removed. They’re less expensive but don’t offer the same stability or feel as fixed options.
3-on-6 sits toward the top of the full-arch hierarchy in terms of stability and biomechanical soundness — but it also requires more bone and a higher implant count, which affects both candidacy and cost.
Treatment is conducted in stages and typically spans several months from first consultation to final restoration.
Assessment and planning: A cone beam CT scan maps your jawbone volume, density, and anatomy in three dimensions. This is used to plan precise implant positioning across the arch and identify whether any preparatory work is needed.
Preparatory treatment: If active gum disease is present, it must be treated and stabilised before surgery. Bone grafting may be required in areas where volume is insufficient to anchor implants securely. These steps add time but are essential for long-term success.
Implant placement: All six posts are placed surgically under local anaesthesia, often in a single session. Sedation is available at most practices for patients who prefer it. A temporary restoration is usually fitted the same day or shortly after, so you leave the appointment with functional teeth.
Osseointegration: Over the following three to six months, the jawbone fuses to the titanium posts through a process called osseointegration. This is what gives the implants their permanent stability.
Final restoration: Once osseointegration is confirmed, the three permanent bridge sections are fabricated and fitted. These are custom-made to match natural tooth colour and anatomy, adjusted for bite, and fixed in place.
Adequate bone volume across the arch Six implants require sufficient bone at six distinct sites. This is a higher bar than single-tooth implants or even All-on-4, where angled placement allows surgeons to work around areas of lower density. If bone loss has occurred — which is common in patients who have been missing teeth for some time — grafting at one or more sites may be necessary. This isn’t automatically disqualifying, but it adds a stage to treatment.
Gum disease under control Periodontitis is a direct contraindication for implant surgery. The bacterial environment created by active gum disease compromises osseointegration and significantly raises the risk of peri-implantitis — an implant-specific inflammatory condition that can lead to bone loss and implant failure. If periodontal disease is present, your provider will want it fully treated and stable before any implant work begins.
General health factors Uncontrolled diabetes slows healing and raises infection risk. Bisphosphonate medications — used to treat osteoporosis — can affect how bone responds to surgery and are an important factor to disclose. Autoimmune conditions and immunosuppressive medications are also relevant. Smoking significantly impairs healing at every stage and is associated with higher implant failure rates; most providers will raise this directly.
Realistic expectations about timeline 3-on-6 is not a quick fix. From initial consultation to final restoration, most patients are looking at six to twelve months, sometimes longer if preparatory treatment is needed. Patients who need results quickly or who are not in a position to commit to the full process may be better suited to a different approach in the short term.
When placed in appropriate candidates and maintained well, implant-supported fixed restorations have an excellent long-term track record. The 3-on-6 design in particular — with its broader implant base and segmented bridgework — is considered biomechanically durable. Individual bridge sections can be repaired or replaced if needed without disturbing the implant posts themselves, which simplifies future maintenance.
Good oral hygiene, regular professional cleaning, and not smoking are the main factors within a patient’s control. With these in place, the restoration can be expected to last many years, and the implant posts themselves often last a lifetime.
If full-arch tooth replacement is something you’re exploring, a consultation with a periodontist or oral surgeon is the place to start. They’ll assess your bone volume, gum health, and medical history to determine which approach suits your situation — and whether 3-on-6 specifically is the right fit or whether a different configuration would serve you better.
The goal is always a restoration that’s stable, comfortable, and built to last. For many patients, 3-on-6 delivers exactly that.